The human papilloma virus (HPV) attacks epithelial cells and has a particle diameter of 55 nm. A special feature is the proliferation of the epithelium of the skin and mucous membranes. In the initial stage, the pathogen usually attacks the basal cells of the epithelium and penetrates them through microtrauma. Localized papillomas are most often found on the skin of the neck, armpits, groin and genitals (most often), oral mucosa and nasopharynx.
This virus can persist for many years without symptoms. Electron microscopic or molecular hybridization methods are used to detect HPV.
Types of human papillomavirus
In humans there is HPV, which affects the mucous membranes and skin. Among the variety of papilloma viruses, types with low and high oncogenic risk are distinguished. It has been proven that oncogenic properties are associated with the ability to integrate DNA into the genome of human cells.
The virus is activated in 10-20% of cases. Depending on the type, benign or malignant changes can occur. Some HPVs are not oncogenic. They lead to the development of warts and genital warts. The most common are HPV 6 and 11.
HPV oncogenes carry a high risk of developing cancerous lesions, particularly on the cervix or anus. HPV 16 and 18 as well as 5 and 8 are more common on the skin and can lead to skin cancer. The most well-known type of cancer caused by HPV is cervical cancer. But men can also become infected with the papilloma virus, which in the worst case scenario causes cancer of the penis or anus.
Women often encounter HPV 16 - this is a form in which introsomal parasitism is observed, i. e. outside the cell chromosome (benign). HPV 18 has a high risk of developing cancer - initially benign tumors form, which after some time degenerate into cancer. In this case, virions have tiny sizes (up to 30 nm).
- neoplasms of the cervix;
- invasive or preinvasive oncology;
- Genital warts of the urinary tract and genitals.
Features of infection

The human papilloma virus is highly contagious. Transmission usually occurs through direct skin-to-skin or mucous membrane-to-mucosal contact with an infected person. Genital infection most commonly occurs during vaginal or oral sex. A large number of sexual partners or other sexually transmitted infections (STIs) increase the risk. Indirect transmission through objects, contaminated clothing or bedding is also possible, but rather rare.
In 7% of cases, transmission of the virus from mother to child can occur during birth if the infection is active. If you are infected with HPV 16 or 18, the risk increases to 40%.

By penetrating the epithelium and violating its integrity, papillomavirus infection promotes the growth of the lower layer of epithelial cells in the form of condyloma or warts. This form of the disease is contagious and spreads quickly to others. Warts and condylomas usually do not cause metastases and often disappear spontaneously.
HPV symptoms
The incubation period is up to 9 months (average 3 months). HPV can be present in the body without any obvious symptoms. The virus can go undetected for months or years. Even at this stage it is contagious.
Skin warts usually appear in groups and increase in number when scratched. The two most common forms of papillomas are either grayish, hard, raised with a broken surface (common wart), or flat and reddish (flat wart). Spiked warts arise on the soles of the feet or heels, grow inwards and are therefore often painful.
- Genital warts. Pale or reddish nodules that often occur in groups and appear on the labia, vagina, penis, urethra, anal canal, and rectum. They are highly contagious.
- Flat condylomas. They appear in the form of flat nodules and occur mainly on the female genital organs. They increase the risk of developing cancer.
- Giant condylomas (Buschke-Levenshtein tumors). They grow into huge formations and destroy the surrounding tissue. In rare cases, they can degenerate and lead to squamous cell carcinoma.
An infection of the mucous membranes of the upper respiratory tract is also possible. The conjunctiva of the eyes may be affected, resulting in pink stalked growths.
It is more difficult to recognize an asymptomatic course, which the doctor can only detect with the help of tools such as acetic acid (causes discoloration of the warts) or a microscope.
In addition, the virus can colonize cells without causing tissue changes. This is then referred to as a latent infection, i. e. the presence of pathogens but no symptoms. After infection, this phase can last from several weeks to several months.
Possible consequences
During an infection, viruses penetrate the cells of the skin and mucous membrane tissue, settle in the cores of cellular structures and multiply there. Typically, such HPV infections go unnoticed and heal on their own without consequences because the immune system successfully fights the pathogen.
However, some types of HPV cause skin changes called growths. Possible forms are genital warts or condylomas and papillomas, which can affect the face, arms or legs, for example.
The resulting tissue changes are usually benign, but can also degenerate and lead to cancer. For example, cancer can occur decades after an HPV infection. Cancers of the external female genital organs (vulvar and vaginal cancer), anal cancer, penile cancer and mouth and throat cancer (tumors in the head and neck area) are also possible.
Establishing the diagnosis

As part of preventative visits to the gynecologist, women are tested for HPV infection. During a gynecological examination, a smear is taken from the cervical lining; this is called a Papanicolaou test (cytological examination). The resulting material is examined for tissue changes to determine precancerous conditions.
In addition, an HPV test can be carried out, in which cell material from a mucous membrane swab or a tissue sample is examined in the laboratory for the presence of certain viruses. However, this only proves that the affected area is infected, but does not say whether tissue changes have occurred. An HPV test is therefore particularly useful in combination with a Pap test and can help detect precancerous lesions at an early stage.
If the test is positive, there is no need to worry as infections do not always lead to cancer. In order to detect tissue changes at an early stage, regular examinations are recommended. Conversely, a negative test result does not say whether there was an infection in the past that the body successfully fought off.
There is no preventive examination for men where the test is carried out regularly. If there is underlying cancer, an examination of the tumor can determine whether the cancer is caused by an HPV infection.
Special DNA methods are also used in laboratory diagnostics, such as real-time PCR. Anogenital warts, caused by HPV types 6 and 11, are easily detected during a pelvic exam.
How to cure human papillomavirus

In most cases, the disease does not require treatment because it goes away on its own and the viruses can no longer be detected. However, if this is not the case, the infection can last longer and last for months or years.
To date, there are no methods of systemic influence on this virus that could completely destroy it. However, treating existing warts reduces the number of viruses, so that in many cases the immune system can fight off and get rid of the remaining viruses. In some cases, the pathogens survive and can cause symptoms of the disease again and again.
- Plantar and genital warts can be treated with medications containing topical salicylic acid.
- Cryotherapy is also a commonly used method for HPV. In this case, the wart is burned with cold and liquid nitrogen.
- Laser or electrocautery are equally used methods.
Cancer caused by HPV is much more difficult to treat. In the case of cervical cancer, it is often advisable to remove the uterus or the upper part of the vagina and the ovaries. This may be supplemented with radiation therapy to eliminate the possibility of a relapse. Other cancers caused by HPV are most often treated with targeted therapies such as radiation or chemotherapy.
It should be borne in mind that surgery is not a radical solution, but only solves a cosmetic problem, since after removal the virus may remain in the surrounding tissues and condylomas may recur.
Infection prevention
There are two vaccinations: a bivalent vaccination against HPV 16 and 18 and a quadrivalent vaccination against HPV 6, 11, 16 and 18. The vaccination is recommended for all young girls aged 14 and over.
A vaccination does not protect against all HPV types. Therefore, all women aged 25 to 65 are advised to have regular smear tests, even if they have been vaccinated.
Timely detection and complete removal of condyloma reduces the risk of the disease. The effectiveness of using condoms to protect against the transmission of infections can significantly reduce the risk of developing this disease. The most promising way to prevent and treat the initial stages of the disease caused by this infection is a specific polyvalent vaccine.
Why plantar warts appear and treatment methods
Warts are skin lesions that appear in the form of special round formations protruding above the surface. They are caused by certain viruses.
Due to their location, these formations often cause physical discomfort. They often recur even after treatment.
Types and reasons
There are many types of warts; they are classified according to a number of characteristics:
- Simply. They appear on exposed parts of the body, arms, legs, face and scalp. They are usually not dangerous, but are not aesthetically pleasing and can multiply quickly and affect large areas of skin. They are arranged like "families".
- Plantar. Their localization is exclusively on the feet. Causes discomfort when walking.
The main cause is infection with the human papilloma virus, which affects mucous membranes and skin.
Human papilloma viruses
This is one of the most common viruses on earth. Infection can occur in different ways:
- contact and household (through touch);
- sexual (genital, anal, oral-genital);
- at birth from mother to child.
The period of development of the disease ranges from several weeks to tens of years. This is explained by the fact that the virus may not manifest itself for a long time, but as soon as the immunity weakens a little, growths immediately appear on the skin and / or mucous membranes. The main danger of this disease is that certain types of HPV have a high probability of causing the formation of a malignant tumor (skin or mucous membrane cancer). To ensure that the disease does not lead to the formation of a tumor, a medical examination and not self-medication is required.
Symptoms and types of warts on the foot
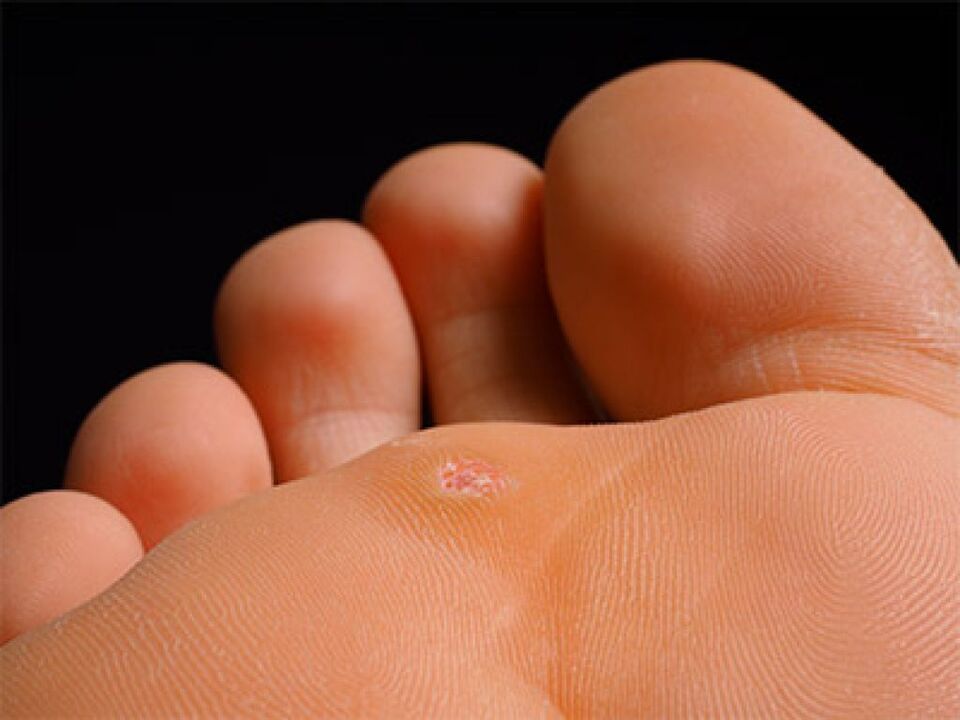
A plantar wart appears as a callus-like thickening with a stratum corneum layer of skin. It hinders walking and causes pain. The passive state is characterized by slow reproduction that does not reach the stratum corneum of the epithelium, so this condition does not manifest itself externally.
The active state is characterized by the fact that the virus develops quickly and manifests itself in numerous symptoms as it rises to the upper layers of the epidermis. The plantar wart is also called plantar wart or chicken wart. The virus penetrates the outer layer of skin through cuts and abrasions upon skin contact:
- First, a small yellowish-gray papule with an uneven surface appears.
- Gradually the small element becomes denser and takes on a dirty color.
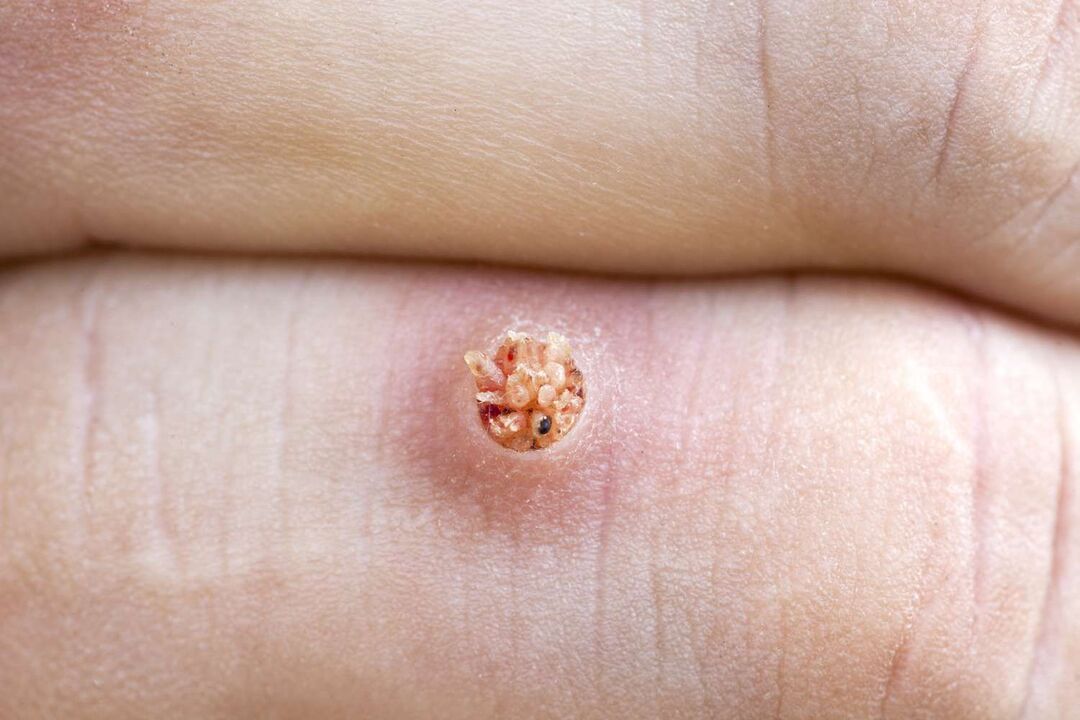
From the inside, a plantar wart looks like overgrown papillae of different sizes with a pink tint. Additional capillary vessels form there, which can lead to bleeding in the event of a wart infection.
Removal of plantar warts
It is worth treating a plantar wart if:
- There are painful sensations.
- The wart is bleeding.
- There were stains on it.
- The wart quickly increases in size.
There are many treatment methods. One of them is cryodestruction. The purpose of the method is to expose the wart to liquid nitrogen at a temperature of minus 196 degrees. The area affected by the virus is frozen and the wart is removed.
The usual and aggressive exposure method is used. The aggressive method involves applying nitrogen for a few seconds longer, but this method is more painful. It is important to note that if a wart appears and persists for more than six months, the effectiveness of cryodestruction decreases sharply and, accordingly, the importance of such an operation also disappears.
After removing a plantar wart with liquid nitrogen, you should follow some recommendations:
- the blister remaining at the site of the wart cannot be opened;
- To avoid mechanical damage, use a sterile bandage instead of a plaster.
- Treat the affected area with 2% salicylic alcohol twice daily;
- Try to prevent water from getting into the affected area.
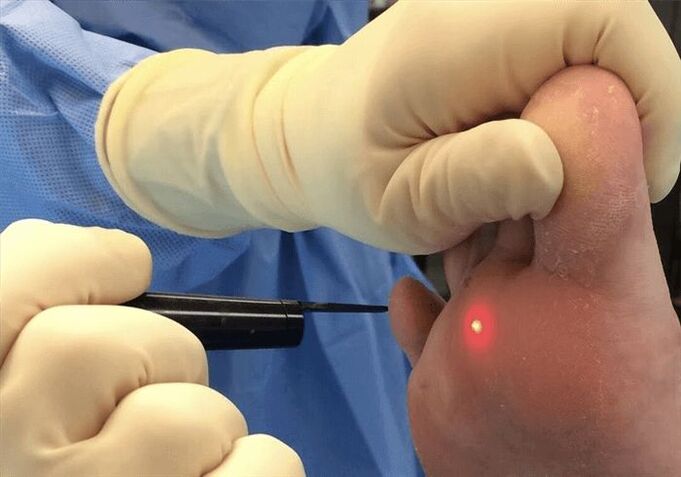
Another method is laser coagulation. This is one of the most common wart removal methods. Most laser systems are equipped with a special cooling system. The procedure therefore takes place with minimal discomfort and does not allow for inflammation as the laser has antiseptic properties. In addition, it is a contactless method.
There are multiple possibilities:
- Carbon dioxide (CO2) laser. In this case, the treatment is carried out using infrared light. The method is 70% effective, but the disadvantage is that healthy tissue can also be damaged.
- Erbium laser. This treatment method uses a shorter wavelength, reducing the likelihood of scarring after surgery. The efficiency is typically 75%.
- Pulsed dye laser. This method of exposure causes primary destruction of the dilated capillaries in the wart and stimulation of the immune system, which contributes to effective healing. The effectiveness of the treatment is around 95%.
After laser treatment, a crust forms on the affected area, which disappears on its own within seven to ten days. The recommendations for this method of treatment are the same as after exposure to nitrogen: avoid mechanical damage and water ingress.
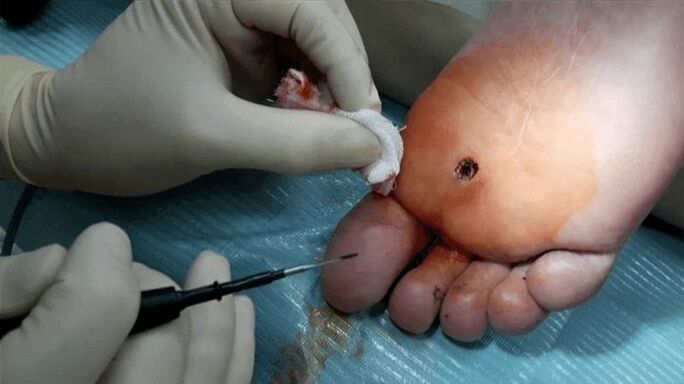
The next option for removing warts is electrocoagulation. A high-frequency current is supplied to the wart. The treatment is carried out under local anesthesia. When a wart is exposed to high temperatures, the cells affected by the papilloma virus evaporate. Another advantage of this method is that it prevents bleeding by cauterizing the blood vessels. After the operation, a crust forms on the affected area of skin, which disappears within 7 to 10 days.
A plantar wart can be treated with direct surgery. In this case, the excision is carried out under local anesthesia and then sutures are applied. After the operation, the doctor will prescribe certain recommendations. Therefore, it is recommended to prevent water and soap from entering the affected area, not to tear off the resulting crust and to treat the affected area with an antiseptic in the first 7-10 days.
There are certain contraindications for each type of surgery. Therefore, the operation cannot be performed if the following occurs:
- Pregnancy;
- diabetes mellitus;
- malignant tumors in the body;
- infection and inflammation around the wart;
- exacerbation of herpes;
- high temperature.
If your blood pressure is high, the procedure should also be postponed.
Treating warts without surgery

People often wonder how to remove a plantar wart without surgery. For this you can use pharmaceutical ointments and solutions.
Basically, these ointments have the following effects:
- anti-inflammatory;
- Antiseptic;
- immunomodulatory;
- antiviral;
- antifungal.
In addition, it may contain vitamin E, which also has a positive effect on treatment, as vitamins generally strengthen the body and reduce the risk of relapse.
It is important that these products are used on single and flat plantar warts. If side effects occur, it is necessary to wash off the medication with plenty of warm water and consult a doctor immediately.
So it is possible to cure warts, there are many ways to do it, but you should not do it without first consulting a doctor so as not to harm your health. In addition, self-medication is strictly prohibited if the attending physician prescribes contraindications.
Treatment of papillomas on the body
Hardware methods
Modern hardware methods of treating papillomas make it possible to get rid of them and prevent the development of a relapse of the disease. The most commonly used methods are:
- Cryodestruction is the destruction of growths by exposing them to low temperatures.
- Electrocoagulation is the cauterization of formations using electric current, the strength and frequency of which is selected depending on the size, type and density of the papilloma.
- Laser removal. The type of effect is clear from the name. The procedure lasts no more than 15 minutes and helps to get rid of unpleasant growths forever.
Medication
The drugs used include celandine, castor oil, lapis pencil, Sani Skin and Dermavit preparations.
They show varying effectiveness and do not prevent relapse of the disease. The main disadvantage of drug therapy for papillomas is the frequent development of allergic reactions.
Prevention of papillomas
To avoid the appearance of growths and infection with human papillomavirus, you should:
- Use barrier contraceptives during sexual intercourse.
- Observe the rules of personal hygiene and use only individual towels, soap and a toothbrush.
- When visiting public pools, don't forget to wear rubber shoes.
In addition, you should normalize your daily routine, eat a balanced diet, give up bad habits and avoid stressful situations. These factors are not the cause of the disease, but can trigger its development if the virus is already present in the body.













































































